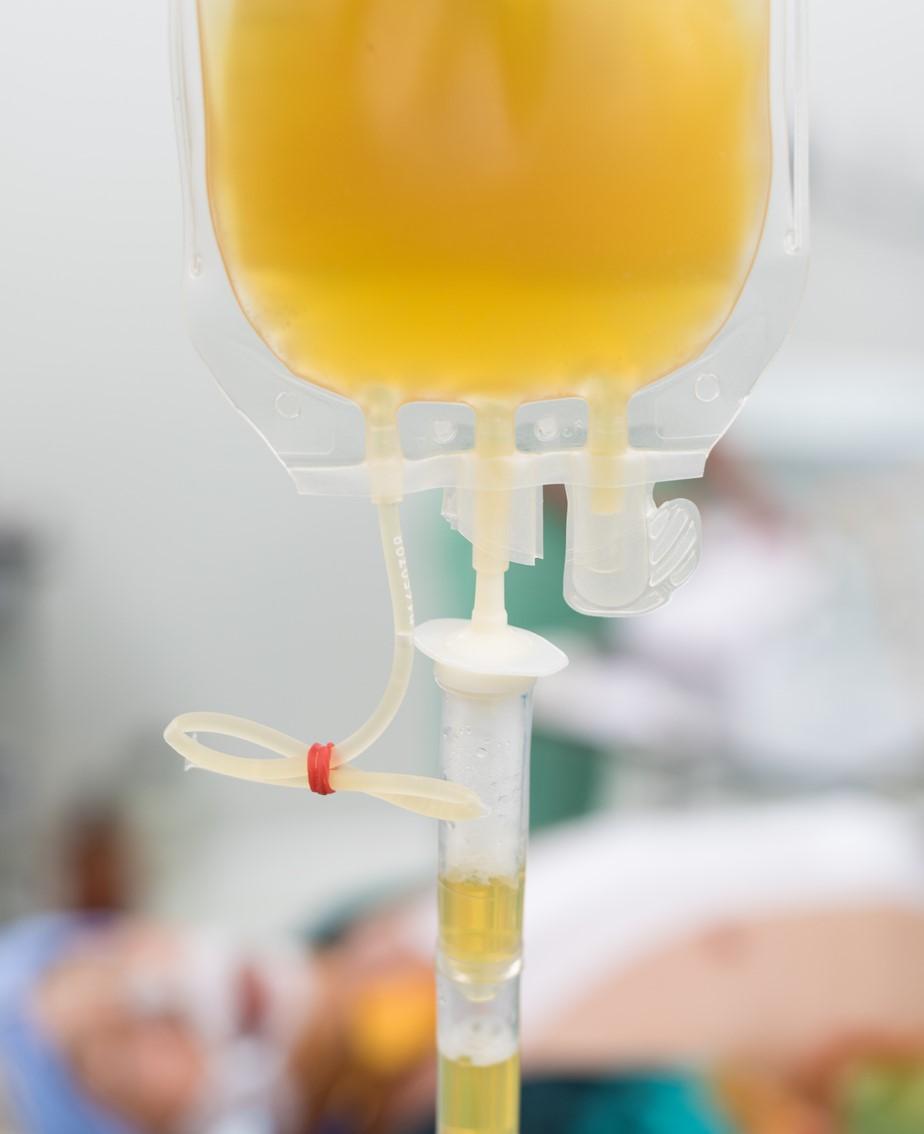
Administration of antibody-rich convalescent plasma to adult patients hospitalized with COVID-19 who did not require mechanical ventilation was linked to a lower risk of death than transfusion of plasma with lower antibody concentrations, according to a study published today in the New England Journal of Medicine.
Led by researchers at Mayo Clinic in Rochester, Minnesota, the retrospective cohort study used a US-wide registry of adult COVID-19 patients from 680 hospitals and determined the levels, or titers, of anti–SARS-CoV-2 immunoglobulin G (IgG) antibodies in plasma donated by recovered COVID-19 patients and transfused into study participants through Jul 4, 2020. The blood-collection centers, researchers, and study participants were blinded to the antibody concentrations at the time of transfusion.
Among the 3,082 patients included in the analysis, all of whom had at least one risk factor for severe coronavirus outcomes, 830 (26.9%) died. One-hundred-fifteen of 515 patients (22.3%) who received high-titer plasma died within 30 days after transfusion, compared with 549 of 2,006 patients (27.4%) given medium-titer plasma, and 166 of 561 (29.6%) given low-titer plasma.
Of the 3,082 patients, 2,014 did not need mechanical ventilation before plasma transfusion. In this subgroup, 50 of 352 (14.2%) who received high-titer plasma died within 30 days, as did 251 of 1,297 patients (19.4%) who received medium-titer plasma, and 81 of 365 patients (22.2%) given low-titer plasma.
That means that patients not receiving mechanical ventilation given high-titer plasma had a 34% lower risk of death within 30 days of transfusion than those receiving low-titer plasma (relative risk [RR], 0.66).
No benefit in patients on mechanical ventilation
In contrast, convalescent plasma given to the 1,068 COVID-19 patients receiving mechanical ventilation did not appear to change the risk of death (RR, 1.02). In this subgroup, 64 of 158 patients (40.5%) in the high-titer group died within 30 days, versus 277 of 666 patients (41.6%) in the medium-titer group, and 80 of 183 (43.7%) in the low-titer group.
The mean time between COVID-19 diagnosis and plasma transfusion was 10.0 days for patients who received mechanical ventilation before transfusion—nearly twice that of patients who did not require mechanical ventilation. The unadjusted death rate within 30 days of transfusion was lower in patients who received their transfusion within 3 days of diagnosis (point estimate, 22.2%) than in those who received theirs later in the disease course (point estimate, 29.5%).
The main variables linked to risk of death within 30 days were, in order of importance, age, signs of severe coronavirus disease (eg, requiring invasive mechanical ventilation, admission to an intensive care unit [ICU]), and antibody concentration.
Of all participants, 61% were men, 23% were black, 37% were Hispanic, and 69% were younger than 70 years.
"These data show that the benefit of convalescent plasma was most apparent in patients who received plasma transfusions containing higher levels of anti–SARS-CoV-2 IgG antibodies early in the disease course," the authors concluded.
Convalescent plasma has been used for more than a century to treat different types of viral respiratory infections. Amid the pandemic, plasma has been administered to COVID-19 patients under the assumption that the antibodies it contains against SARS-CoV-2, the virus that causes COVID-19, can help them fend off severe disease. But whether high antibody levels are linked to a lower risk of death than low antibody levels is under exploration.
On Aug 23, 2020, the US Food and Drug Administration granted an emergency use authorization for the use of convalescent plasma in hospitalized coronavirus patients with signs of worsening infections.
But a National Institutes of Health guidelines panel said, "There are insufficient data for the COVID-19 Treatment Guidelines Panel (the Panel) to recommend either for or against" its use. And the Infectious Diseases Society of America and the AABB (formerly the American Association of Blood Banks) recommend limiting the use of convalescent plasma to clinical trials, noting that critically ill patients are unlikely to benefit and that if plasma is used, it should be done within 3 days after diagnosis to achieve the best results.
Reserving plasma for high-risk patients
A commentary today in the same journal reflects on a Jan 6 convalescent plasma study that found that early transfusion of high-titer convalescent plasma into mildly ill older adults reduced the progression of COVID-19.
In the commentary, Louis Katz, MD, of the Mississippi Valley Regional Blood Center in Davenport, Iowa, noted that previous trials of convalescent plasma in COVID-19 patients have produced mixed results. Observational studies, which cannot prove causation, have been more positive than randomized trials, considered the gold standard of investigations, in terms of the efficacy of convalescent plasma in COVID-19 patients, he said.
Given these results and sometimes-scarce plasma, Katz said that convalescent plasma should be used in only mildly ill older COVID-19 patients, younger patients at high risk for severe disease, and certain immunocompromised patients. All should be treated with high-titer plasma within 3 days of symptom onset, he said.
"Uncontrolled compassionate use of convalescent plasma in patients other than those with an early infection that is likely to progress to more severe illness should be discouraged, even though clinicians recognize how difficult it can be to 'just stand there' at the bedside of a patient in the ICU," Katz said.
"Constraints on therapies for COVID-19 that are effective for limited patient populations are a powerful argument for continued consistent adherence to recommended nonpharmaceutical interventions and the rapid deployment and uptake of effective vaccines," he added.