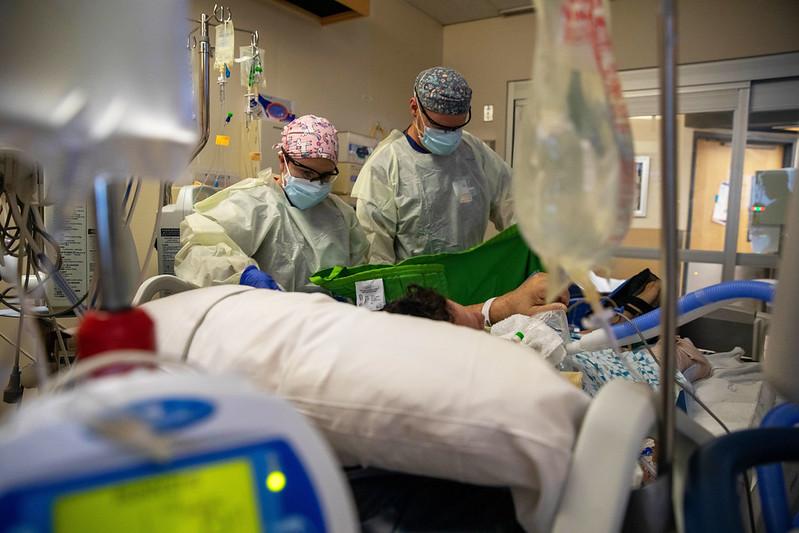
COVID-19 patients' vital signs, lab results, and need for supplemental oxygen when they arrive at the hospital can better predict illness severity than underlying illnesses and differ by age-group, suggests a modeling study published today in Scientific Reports.
A team led by Institute for Systems Biology in Seattle led the study to improve risk stratification for hospitalized COVID-19 patients, a process important for clinical decision-making and resource allocation.
Delta dominated study period
The researchers retrospectively analyzed the electronic health records from 6,906 adults hospitalized with COVID-19 from a community health system with 51 hospitals and 1,085 clinics in Alaska, California, Montana, Oregon, and Washington from Jun 30 to Nov 15, 2021, a period dominated by the Delta SARS-CoV-2 variant. Most hospitalized patients (92% of those younger than 50, 75% of older patients) hadn't been vaccinated against COVID-19.
Using clinical data from the first hour of either hospital admission or positive COVID-19 test, the team built models to predict the need for mechanical ventilation or death in the next 56 days. Patients were classified as younger than 50 years (1,963 patients) or 50 and older (4,943). Average patient age was 60 years, and 44.3% were women.
Aggregated vital sign values from 24 hours before to 1 hour after included average heart rate, systolic and diastolic blood pressure, respiratory rate, blood oxygen saturation, and body temperature.
The risk-prediction models for within 7 days of hospitalization or diagnosis had an under-the-receiver operating characteristic (AUROC) of 0.81 for younger patients and 0.82 for the older group, indicating excellent performance.
Critical illness or death occurred in 10.9% of patients (7.8% of younger patients, and 12.0% in older group). In both age-groups, aggregated vital signs, lab tests, and the need for supplemental oxygen better predicted poor COVID-19 outcomes than underlying conditions or demographic factors such as sex.
Need to update early risk-prediction models
"Age stratification shows that risk factors for severe COVID-19 differ by age, in ways that cannot be determined in all-age models," the researchers wrote. "This affirms the importance of analyzing each different age group separately, particularly for the older population who have the greater overall risk for poor outcomes."
Other risk factors for critical illness and death in the younger group were higher body mass index (BMI), older age, and the presence of heart failure and/or cardiomyopathy (impaired ability to pump blood to the rest of the body). Predictive individual lab values included higher aspartate aminotransferase (AST) and creatinine levels and lower calcium levels.
Lab results were more important for older than younger patients. Additional risk factors in the older age-group included higher BMI, older age, the presence of dementia, and the use of vasopressors (drugs to raise blood pressure) within 1 hour of hospital admission or COVID-19 diagnosis.
BMI was a more important predictor of COVID-19 severity for younger rather than older patients, as were underlying illnesses such as cancer and chronic obstructive pulmonary disease (COPD).
Among older patients, predictive individual lab risk factors included higher blood urea nitrogen and AST levels and lower bicarbonate and calcium levels.
"Our models show that chronic conditions, comorbidities, sex, race and ethnicity are much less important in the hospital setting for early prediction of critical illness," lead study author Sevda Molani, PhD, said in an Institute for Systems Biology news release.
Coauthor Jason Goldman, MD, MPH, of the Swedish Center for Research and Innovation in Seattle, said that risk prediction is complex because the COVID-19 disease course varies widely, from asymptomatic to critical illness or death.
"While age is known to be highly predictive of death, other risk factors within age strata are incompletely explored," Goldman said in the release. "These findings remind the treating clinician to incorporate physiological parameters into risk stratification, and subsequently into decisions on treatment allocations."
Corresponding author Jennifer Hadlock, MD, of the Institute for Systems Biology, said that risk models developed early in the pandemic need to be updated to reflect current COVID-19 standards of care, in which fewer uncommon lab tests are used and more treatment options are available. "As the standards of care for COVID-19 evolve, our risk models need to evolve with them," she said.