- The United Kingdom–based Wellcome Sanger Institute Genomic Surveillance Unit (GSU) and South Africa's Stellenbosch University Centre for Epidemic Response and Innovation (CERI) today announced a new partnership to coordinate global genomic surveillance of infectious diseases. In a statement, Tulio de Oliveira, PhD, who founded and leads CERI and led the group's work that identified the Omicron SARS-CoV-2 variant, will also join GSU as its deputy director. "Between our two teams, we can share complementary facilities and work together on many diseases: from those carried by mosquitoes or floodwaters, to respiratory viruses with pandemic potential," he said. de Oliveira praised the two groups' staff and their ability to attract support from funders and governments. "We are in a good position now to respond effectively to epidemics in our own regions, and support genomic surveillance across the world."
- The National Association of County and City Health Officials (NACCHO) announced today that it will award $1.29 million to 17 public health departments in 11 states to boost healthcare infection prevention and control and antimicrobial stewardship efforts. The selected local health departments will use the funding to conduct infection control assessments, strengthen antimicrobial stewardship programs, and build strategic approaches to reducing healthcare-associated infections (HAIs)—including those caused by antibiotic-resistant pathogens. The Centers for Disease Control and Prevention estimates that 1 in 31 patients are infected with at least one HAI during a hospital stay, and several of the leading antibiotic-resistant threats are associated with healthcare settings.
- Four states—California, Kansas, South Carolina, and South Dakota—have reported more avian flu outbreaks in poultry flocks over the past few days, three of them reporting the virus on commercial farms, according to the latest updates from the US Department of Agriculture (USDA) Animal and Plant Health Inspection Service (APHIS). California's outbreak involves a layer pullet farm in Merced County that houses more than 285,000 birds. Kansas reported an event at a gamebird producer in Mitchell County that has 5,800 birds. The virus also struck a gamebird producer in South Dakota, a facility in Mitchell County that has 21,000 birds. In South Carolina, outbreaks involving backyard birds were reported in Horry and Orangeburg counties. The pace of outbreaks appears to have slowed, compared to rapid increases that occurred October through December.
Quick takes: Genomic surveillance partnership, infection prevention and antimicrobial stewardship, more avian flu in US
CDC alerts healthcare providers about measles cases
The US Centers for Disease Control and Prevention (CDC) today urged healthcare providers to be alert for patients who have fever and rashes and have traveled abroad, following reports of 23 measles cases since December 1, 2023.
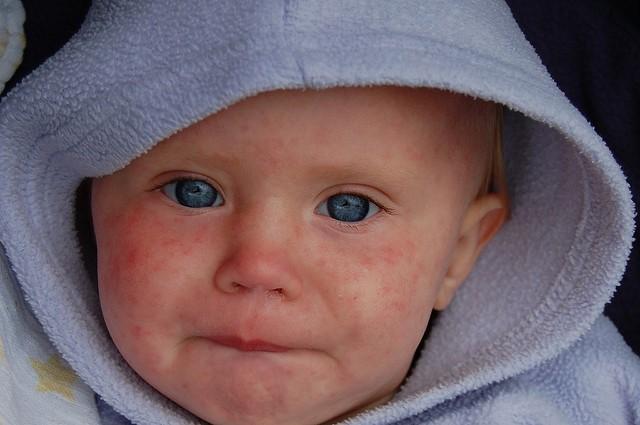
"The increased number of measles importations seen in recent weeks is reflective of a rise in global measles cases and a growing global threat from the disease," the CDC said in an email.
Clusters in Philadelphia, Washington state
Of the 23 cases, 7 were imported cases in international travelers. Also, there have been two outbreaks of more than 5 cases each. One is an outbreak in Philadelphia that led to infections at a hospital and a daycare facility. The other appears to be a family cluster of six cases in Washington's Clark and Wahkiakum counties in the southwestern part of the state.
In other recent developments, Virginia officials warned of measles exposures at two international airports, New Jersey confirmed a case in Camden County, and Georgia reported a case in Cobb County involving an unvaccinated resident of the metro Atlanta area who had recently traveled outside the country.
In its email alert to clinicians, the CDC said most of the cases involve young children and adolescents who had not received a measles-containing vaccine, even though they were eligible.
Antibiotics and reflux drugs, when combined, linked to increased C diff risk
A population-based study in Sweden found that recent use of antibiotics and proton pump inhibitors (PPIs)—drugs often used to relieve acid reflux—was associated with increased risk of Clostridioides difficile infection (CDI), particularly when used in combination, researchers reported yesterday in the Journal of Antimicrobial Chemotherapy.
While the use of antibiotics and PPIs have each been independently associated with increased risk of CDI in several studies, few studies have investigated the potential effects on CDI risk when used in combination. To do so, a team led by researchers at Sweden's Karolinska Institutet compared all 43,152 CDI patients diagnosed in Sweden from 2006 through 2019 with 355,172 matched population controls without CDI, assessing the impact of recent (0 to 30 days) and preceding (31 to 180 days) use of antibiotics and PPI on CDI and recurrent CDI risk.
Higher risk for recent use
Overall, 63% and 39% of patients with CDI were at some point exposed to antibiotics and PPIs before infection, respectively, compared with 16% and 14% of controls. When recently exposed to both, the odds for CDI were 17.51 (95% confidence interval [CI], 17.48 to 17.53) higher than among those not exposed, while the odds ratio [OR] was 15.37 (95% CI, 14.83 to 15.93) for antibiotics alone and 2.65 (95% CI, 2.54 to 276) for PPI alone. The effect of preceding use was less pronounced, with an OR of 9.13 (95% CI, 8.71 to 9.57) for combined use, 5.42 (95% CI, 5.26 to 5.57) for antibiotics alone, and 2.08 (95% CI, 2.01 to 2.15) for PPI alone.
While recent antibiotic use resulted in slightly higher odds of recurrent CDI (OR, 1.30; 95% CI, 1.23 to 1.38), recent PPI use was not associated with CDI recurrence (OR, 1.03; 95% CI, 0.94 to 1.12), and the combined effect was no different than the effect of antibiotics alone. Recent macrolides/lincosamides/streptogramins, other antibacterials including nitroimidazole derivates, non-penicillin beta lactams, and quinolones showed the strongest association with CDI risk and recurrence, particularly for recent use.
"Our findings stress the need to reconsider the risk-benefit of both antibiotics and PPIs, which are both still over-prescribed," the study authors wrote.
Global flu activity slows
Though flu is still rising in some Northern Hemisphere countries, the overall global trend declined as 2023 ended and into the first week of the new year, the World Health Organization (WHO) said in its latest update.
Activity increased in Europe and Central Asia, along with sharp rises in hospitalizations and intensive care unit admissions. Flu activity also rose in parts of North Africa, except in Egypt. Central America and the Caribbean also reported further rises in flu detections.
Illness activity remained elevated in North America, mainly due to the 2009 H1N1 strain. Though flu activity remained elevated in East Asia, activity showed an overall decline owing to decreased detections in China and South Korea. Hong Kong and Mongolia, however, reported increasing trends. Southeast Asia's flu activity is still elevated, mainly due to the H3N2 strain.
Flu activity declined on the Arabian Peninsula, as well as in South Asia.
Elsewhere, detections declined in South America's tropical regions, except for Colombia and French Guiana. Little flu activity was reported in South America's temperate countries, except for Chile.
Of respiratory samples that tested positive for flu at national flu labs during the reporting period, 84.2% were influenza A. And of subtyped influenza A viruses, 73% were H3N2.
Childhood obesity rates soared in UK during COVID-19

Yesterday in PLOS One researchers from the University of Southampton showed that obesity rates for British preschoolers in 2020 and 2021 skyrocketed more than 45% compared to 2019 and 2020.
The authors said this is the largest single-year increase in overweight and obesity prevalence in recent UK history, and will result in an additional £800 million ($1 billion US) in healthcare costs for now-overweight children who will likely suffer chronic diseases.
The study was based on publicly available annual body mass index (BMI) data from 2006 through 2022. Two age-groups were studied, kids ages 4 to 6 years old and 10 to 11.
Obesity prevalence among children ages 4 to 5 years increased by 45% during the first year of the pandemic; from 9.9% in 2019 to 2020 to 14.4% in 2020 to 2021. The prevalence then decreased to 10.1% in 2021 and 2022, returning to the pre-pandemic trend, the authors said.
Lower-income kids more likely to be obese
While weight for children ages 4 and 5 rebounded to healthy BMIs by 2022, obesity in children ages 10 to 11 persisted and was 4 percentage points higher than expected, representing almost 56,000 additional children who were now clinically overweight.
Children in both age-groups who were from low-income homes were more likely to have higher BMI. There was no difference, however, among BMI rates across different ethnic groups.
"The sharp increase in childhood obesity during the COVID-19 pandemic illustrates the profound impacts on children’s development," said Keith Godfrey, PhD, a co-author of the study, in a PLOS press release. "Alongside the escalating costs of the ongoing epidemic of childhood obesity, it is clear that more radical new policy measures are required to reduce obesity and secure wellbeing and prosperity for the country as a whole
Closing toilet lid before flushing doesn't keep viral spray inside, study suggests

Contrary to previous study findings, closing the toilet lid before flushing doesn't stop aerosolized viruses from contaminating bathroom surfaces, scientists from the University of Arizona and Reckitt Benckiser LLC, the company that makes the disinfectant used in the study, report in the American Journal of Infection Control.
The researchers added a bacteriophage (virus that targets and kills bacteria) to household and public toilet bowls as a proxy for human intestinal viruses. After they flushed the toilets (with the lid open or closed in case of the household toilets), they measured viral contamination of the toilet and bathroom floor and walls.
"Research has demonstrated that people with COVID-19, even those who are asymptomatic, excrete severe acute respiratory syndrome coronavirus (SARS-CoV-2) in fecal matter and other excretions," the researchers wrote. "Viruses contaminating urine and feces can be aerosolized in building restrooms during toilet flushing."
The resulting toilet aerosol plumes, they said, can land on surfaces more than 5 feet away.
Bowl disinfection slashed contamination
The amount of virus collected from surfaces on the household toilet or floor wasn't significantly different whether the lid was open or closed. The toilet seat had the most contamination, while walls had little. Comparable contamination patterns were noted with the public toilet.
With results showing that closing toilet lids has no meaningful impact on preventing the spread of viral particles, our study highlights the importance of regular disinfection of toilets to reduce contamination and prevent the spread of viruses.
Brushing the toilet bowl with Lysol Power Toilet Bowl Cleaner reduced contamination of bowl water (vs no disinfectant) by over 99%. Contamination of the bowl brush was 98% lower when Lysol was used. Adding Lysol to the bowl before flushing or using disinfectant dispensers in the tank helped lessen flushing-related contamination.
In a news release from the Association for Professionals in Infection Control, publisher of the journal, senior author Charles Gerba, PhD, of the University of Arizona, said the results are important for preventing pathogen transmission in healthcare settings. "With results showing that closing toilet lids has no meaningful impact on preventing the spread of viral particles, our study highlights the importance of regular disinfection of toilets to reduce contamination and prevent the spread of viruses," he said.
The study was funded by a grant to the University of Arizona from Reckitt Benckiser.













