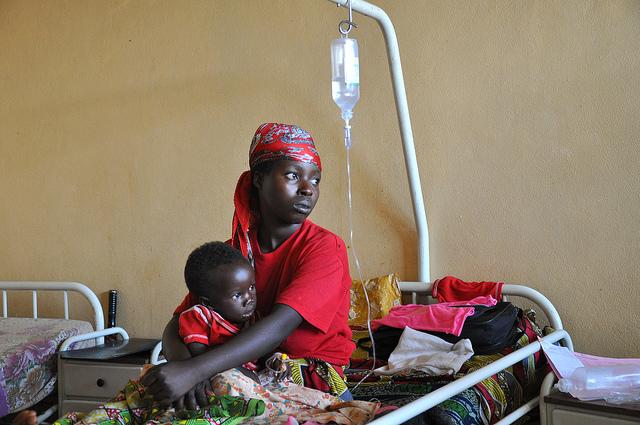
Two major malaria conferences under way this week—one in London and the other in Senegal—brought new pledges of nearly $4 billion to curb the disease and new research on factors that are driving disease levels, such as conditions in conflict zones and contaminated blood supplies.
As part of the Commonwealth Heads of Government Meeting in London this week, leaders the countries attended a Malaria Summit today that was cohosted by Rwanda, Swaziland, and the United Kingdom. During the event, donors announced new funding for research and development, and countries that are part of the group were urged to halve malaria across the Commonwealth by 2023.
Meanwhile, the 7th Multilateral Initiative on Malaria Pan African Malaria Conference is under way in Dakar, Senegal, this week, where researchers unveiled new findings about the spread of the disease.
London summit galvanizes support
In London, new donor commitments were led by an additional $1 billion from the Bill & Melinda Gates Foundation, $2 billion from the Global Fund to Fight AIDS, Tuberculosis, and Malaria, and pharmaceutical companies Glaxo Smith Kline ($250 million) and Novartis ($100 million), Bloomberg News reported.
Pledges also came from countries, such as the United Kingdom, which announced a $1.42 million grant to be matched by the private sector to help supply priority countries with mosquito nets and indoor sprays, as well as to strengthen healthcare systems.
According to a UK government statement yesterday, malaria is a key issue for Commonwealth countries, of which 90% of citizens live in affected countries. Penny Mordaunt, the UK's international development secretary, said, "We know malaria still causes one out of ten child deaths in Africa and costs economies billions every year. We also know progress on reducing malaria cases has stalled, which is why it is so important it is one of the focuses of the Commonwealth Heads of Government Meeting."
Also, Uganda committed to establish a malaria fund to mobilize $785 million by 2020 to speed up its progress against the disease, according to a press release from the Global Fund to Fight AIDS, Tuberculosis, and Malaria.
Novartis said in a press release yesterday that its $100 million in funding over the next 5 years will target research and developments of next-generation treatments to fight emerging resistance to artemisinin and other antimalarials that are currently used. It also added that it will roll out an equitable pricing strategy to maximize access to the new treatments for patients where the disease is endemic.
Specifically, it said the investment is designed to advance the company's malaria product pipeline through 2023 and to complete global clinical trials for two new antimalarial drug candidates, KAF156 and KAE609, which are currently in phase 2 studies.
Vas Narasimhan, chief executive officer of Novartis, said, "Resistance to treatment presents the biggest threat to the incredible progress that has been made in the fight against malaria in the past 20 years. We cannot afford to wait; this is why we are committing to advance the research and development of next-generation treatments."
Challenges in conflict zones, with blood banks
Meanwhile, experts at the pan-African malaria conference, held every 3 to 4 years, warned that a rapid rise in malaria cases in deaths in countries grappling with conflict and famine could thwart the last 10 years of progress against the disease.
In a press release from the meeting, Richard Allan, with The Mentor Initiative, a nongovernmental organization that works against malaria in countries experiencing humanitarian crises, said, "The global battle against malaria is going to fail unless we get real about where the malaria burden is today and expand the tools and techniques we use to fight it."
At the meeting, researchers presented new information on the scope of the problem and studies that suggest that a mix of tools and tactics can drive down disease levels, even in the chaos of conflict. One team presented World Health Organization (WHO) data showing that, as global malaria deaths dropped sharply over the past 6 years, infections and deaths surged in many areas experiencing armed conflict, including Nigeria, Ivory Coast, South Sudan, and Central African Republic.
Strategies that can be effective, according to studies presented at the meeting, include:
- Establishing a network of community health workers—supplied with backpacks full of supplies—to use rapid diagnostic tests, administer malaria drugs
- Ensuring access to minimal but appropriate care to reduce the number of deaths that occur trying to transport sick patients to medical facilities
- Developing long-lasting insecticide-treated mosquito nets (LLINs) that are treated with a second insecticide that mosquitoes haven't developed resistance against
- Findings safe and effective alternatives to LLINs, such as temporary housing made with insecticide-treated plastic sheeting, with spraying inside living quarters and supplying residents with insecticide-treated blankets
- Helping pregnant women prevent infection by offering mobile clinics, which was done in South Sudan
In other meeting developments, scientists reported new findings on the high risk of malaria transmission after blood transfusions in sub-Saharan Africa, according to a separate press release from the meeting.
In one review, a team looked at results from 24 studies to gauge malaria prevalence among 22,508 blood donors. It found that nearly one in four (23.46%) blood bank supplies contained parasites that cause malaria.
The investigators pointed out that half of all kids receiving blood transfusions undergo the procedure to treat malaria-induced anemia, and that contaminated blood supplies put them and their parents at risk. They added that more research is needed on ways to remove Plasmodium parasites from the blood banks.
Meanwhile, researchers involved in another study that looked at the blood supply of Equatorial Guinea's capital city of Malabo found much higher levels of latent malaria infection, most of it at a level that current diagnostic tests cannot detect. Low-level or asymptomatic infections can hide parasites that have the potential to trigger future malaria outbreaks.
For the study, the researchers used a more sensitive test, quantitative polymerase chain reaction, to examine 200 blood samples. They found that 29.5% of the samples harbored low concentrations of the parasites, though they were thought to be free of them.
See also:
Apr 17 Bloomberg News story
Apr 17 UK government statement
Apr 18 Global Fund press release
Apr 17 Novartis press release
Apr 17 meeting press release on fighting malaria in conflict zones
Apr 16 meeting press release on malaria blood transfusion risk