- Respiratory syncytial virus (RSV) emergency department visits and hospitalizations continue to rise across the United States, and hospitalization rates for the virus are now increasing in seniors, the Centers for Disease Control and Prevention said earlier this week in a respiratory virus snapshot. RSV test positivity is rising steadily but is still below the peak for 2022. The CDC recommends the RSV vaccine for people ages 60 and up, based on shared decision making with health providers, and the CDC estimates that 14.3% of people in that age-group have been immunized.
- Researchers at the Netherlands' Wageningen University have reported that the highly pathogenic H5N1 avian flu virus connected to a recent layer farm outbreak involves a new variant that contains the PB1 gene segment from a low-pathogenic virus, according to a statement translated and posted by Avian Flu Diary, an infectious disease news blog. So far, it's not clear how pathogenic or contagious the variant is in poultry. In other avian flu developments, the US Department of Agriculture reported two more outbreaks in poultry at commercial farms, one at a broiler facility in Oregon and the other on a turkey farm in Minnesota. And animal health officials in Greenland have reported the first appearance of highly pathogenic H5N5 in wild birds, according to a notification from the World Organization for Animal Health. The detections were in a northern fulmar and a gull found dead in Disko Bay in western Greenland.
- Six countries reported more polio cases this week, including Pakistan, which reported its fifth wild poliovirus type 1 (WPV1) case of the year, according to the latest weekly update from the Global Polio Eradication Initiative. The Pakistani patient is from Sindh province. The five other countries, all in Africa, reported more vaccine-derived cases. Chad, the Democratic Republic of the Congo (DRC), Guinea, Nigeria, and Somalia reported more circulating vaccine-derived poliovirus type 2 (cVDPV2) cases. The DRC also reported four more cases involving circulating vaccine-derived poliovirus type 1 (cVDPV1).
Quick takes: RSV climbs in US, H5N1 avian flu variant, polio in 6 nations
US flu activity continues to rise steadily
Positive tests, hospitalizations, and outpatient visits for flu rose again last week, with levels highest in the south central, south, and western regions, the Centers for Disease Control and Prevention (CDC) said today in its latest update.
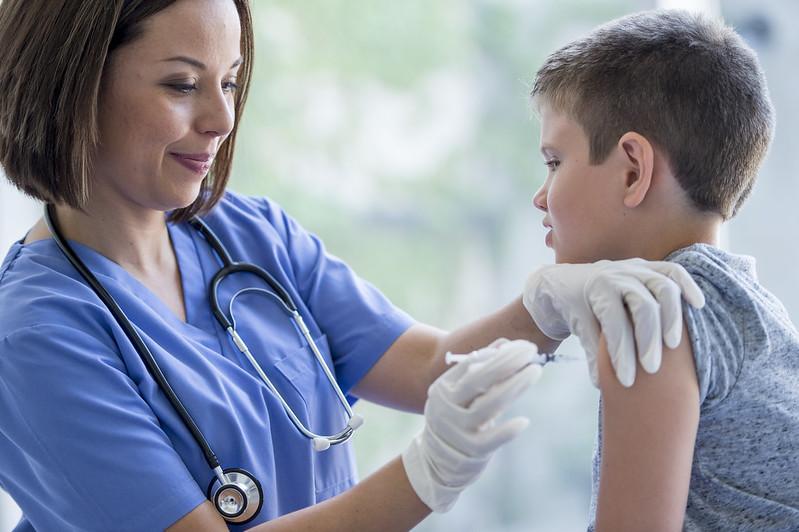
The percentage of outpatient visits for flulike illness, at 3.5%, is above the national baseline for the second week in a row and is at or above baselines in 5 of 10 US regions. The percentage of respiratory specimens that were positive for flu rose to 4%, up from 3% the week before. Among positive samples at public health labs, 75.8% were influenza A, and, of subtyped specimens, 87.2% were the 2009 H1N1 strain.
Estimated 8,000 hospitalizations, 490 deaths
The CDC estimated that there have been at least 780,000 flu infections, 8,000 hospitalizations, and 490 deaths from flu so far this season.
Hospitalizations rates are highest in seniors and in children ages 4 and younger, the two age-groups that also have the highest levels of outpatient visits.
One state—Louisiana—reported very high flu activity, a marker that tracks clinic visits for flu. Eight jurisdictions reported high activity: Alabama, the District of Columbia, Florida, Georgia, Mississippi, New Mexico, Puerto Rico, and South Carolina.
The CDC didn't report any new pediatric flu deaths, which remain at one for the season. Earlier this week, however, Mississippi reported its first flu death of the season.
Regarding flu vaccine uptake, the CDC estimates that more than half (57.6%) of seniors have been immunized, followed by nearly 35% of adults in other age-groups and 32.6% of children. The CDC recommends that all people ages 6 months and older be vaccinated against flu.
High-dose fluvoxamine did not shorten COVID recovery times
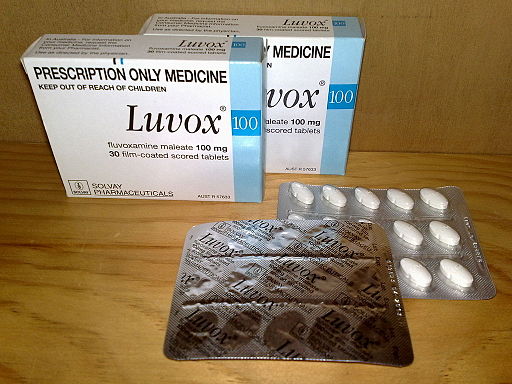
Results from a randomized clinical trial today of 1,208 participants show that high-dose (100-milligram [mg]) fluvoxamine did not improve time to sustained recovery in people with mild to moderate COVID-19 infections.
Fluvoxamine, known as Luvox, is a selective-serotonin reuptake inhibitor. Its potential use for COVID-19 was considered as part of the Accelerating Coronavirus Disease 2019 Therapeutic Interventions and Vaccines (ACTIV-6) platform, which aims to investigate repurposed medications in the outpatient setting for mild to moderate COVID-19.
The study is published in JAMA.
Participants were enrolled from August 25, 2022, to January 20, 2023, and were 30 years or older with confirmed SARS-CoV-2 infection and at least two acute COVID-19 symptoms for 7 days or less. The participants were randomized to receive fluvoxamine 50 mg twice daily on day 1 followed by 100 mg twice daily for 12 additional days (601 patients), or a placebo (607).
The primary outcome was time to 3 consecutive days without symptoms.
All patients recovered in 10 to 11 days
The participants' average age was 50 years old, 65.8% were women, 45.5% identified as Hispanic/Latino, and 76.8% reported receiving at least two doses of a SARS-CoV-2 vaccine.
The authors found no differences among the study participants in time to recovery (adjusted hazard ratio, 0.99; 95% credible interval, 0.89 to 1.09), with both groups achieving sustained recovery by days 10 or 11. No participants died during the study, and fluvoxamine was not associated with any adverse events.
In an editorial on the study, two JAMA deputy editors wrote that the ACTIV trial is a success story of the pandemic. They note that shortly after the pandemic began, "the ACTIV platform also quickly began generating key insights for outpatient management of COVID-19 infection, such as the ineffectiveness of ivermectin."
They suggest the model should be used to investigate treatments to several outpatient diseases in addition to COVID.
Study shows modest flu vaccine protection against serious disease in kids last season
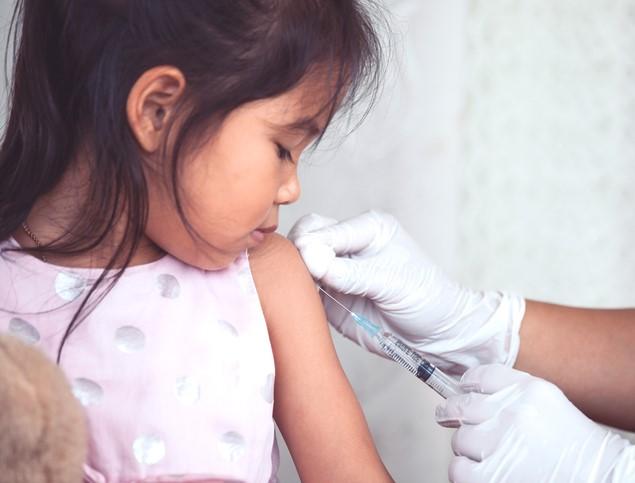
An analysis of US national data finds a flu vaccine effectiveness (VE) against severe outcomes of 48% overall in kids in 2022-23, 53% among preschoolers, and 38% among children aged 9 to 17 years.
The study was published yesterday in Clinical Infectious Diseases. The 2022-23 flu season saw the highest influenza-associated pediatric hospitalization rate in the United States since 2010-11. Most of the illness was caused by the H3N2 strain.
Outcomes were based on pediatric patients seen at 55 hospitals and 107 emergency department (ED) or urgent care (UC) sites through Kaiser Permanente Northern California, Intermountain Healthcare in Utah, and HealthPartners in Minnesota and Wisconsin.
40% protection against hospital cases
The VE for vaccinated children against emergency department and urgent care (ED/UC) visits was 48% (95% confidence interval [CI], 44% to 52%). The study showed that 15.2% of vaccinated kids and 27.1% unvaccinated children made up ED/UC flu patients.
The VE against hospital admission for the flu was 40%. Among kids hospitalized for the flu, 17.5% were vaccinated and 33.4% were unvaccinated. The authors of the study said lower VE may be due to lower vaccine coverage.
The atypically early start of the 2022–2023 influenza season may have resulted in lower observed vaccine coverage.
"The atypically early start of the 2022–2023 influenza season may have resulted in lower observed vaccine coverage, as activity started and peaked before many children and adolescents may have had an opportunity to get vaccinated," they wrote.
MSF details mpox outbreak in DR Congo
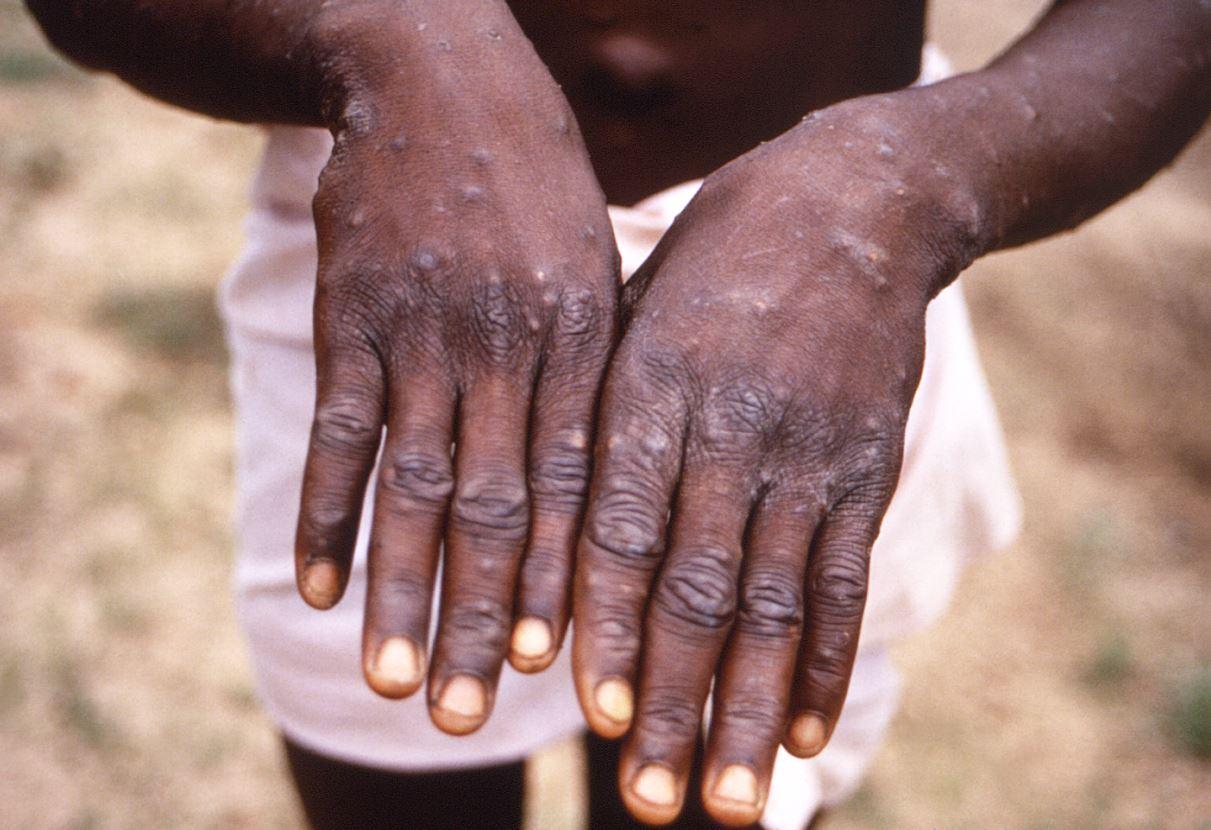
Medecins Sans Fronteires (MSF, or Doctors Without Borders) said yesterday that it battled an mpox outbreak in the Democratic Republic of the Congo (DRC)'s Equateur province from August to mid-October.
An emergency team was in the Bolomba health zone in the western DRC to help health officials treat 890 mpox patients, provide education, contain spread of the virus, support 11 remote health centers, and conduct surveillance. Seventy-two patients (8.1%) were hospitalized.
Mpox, which is characterized by skin lesions, can be accompanied by fever, sore throat, muscle aches, or lymph-node pain.
"If the disease is not treated in time, it can lead to complications and death in those affected, especially if their immune system is compromised by other diseases," Raphael Kibwantiaka, head of MSF's emergency response in Bolomba, said in a news release. "As Bolomba was already grappling with a measles epidemic, we intervened against both diseases."
Measles, malnutrition, malaria
The workers followed up with more than 800 mpox patients at home and organized awareness-raising activities in healthcare facilities and the community to prevent disease transmission and combat stigma, "as the disease has highly visible signs on the body, sometimes leading to the rejection of patients by the community," Kibwantiaka said.
The emergency team vaccinated 110,723 children against measles and treated 3,355 others. They also treated 827 malnourished children and 2,583 with malaria.
The disease has highly visible signs on the body, sometimes leading to the rejection of patients by the community.
Staff sometimes had to travel by canoe or motorcycle, often in the rain. Kibwantiaka said Bolomba's remote, densely wooded environment is rich in wildlife, which makes it conducive for the development of diseases with animal origins, such as mpox.
"Eating bushmeat, handling dead animals, and animal bites or scratches encourage the transmission of the virus from animals to humans," he said. "Infected individuals then become highly contagious and need to isolate themselves quickly to prevent widespread transmission."













