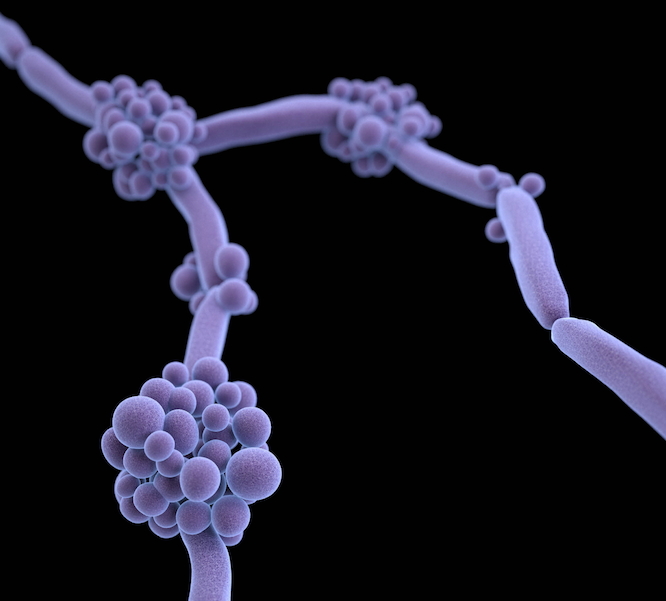
Hospitals in the United Kingdom have detected more than 200 patients colonized or infected with the multidrug-resistant fungus Candida auris, according to a new report from Public Health England (PHE).
Approximately one quarter of the cases, which have been detected at more than 55 hospitals across the United Kingdom, are clinical infections, including 27 patients who developed bloodstream infections. The other patients have not shown any sign of infection, a PHE microbiologist told Reuters. No deaths have been attributed to infection.
The first C auris infection in the United Kingdom was identified in 2013. Since then, there have been three large nosocomial outbreaks in intensive care units in English hospitals. As of yesterday, all three hospitals had declared their outbreaks over, the PHE report says.
C auris was first identified in the ear of a patient in Japan in 2009 and since then has emerged as a serious global health threat because of its growing resistance to azoles, echinocandins, and polyenes—the three classes of antifungals used to treat Candida and other fungal infections. The multidrug-resistant fungus can cause severe invasive infections in immunocompromised patients and has been associated with high mortality. Reports from countries that have documented cases indicate that the majority of patients have multiple underlying health conditions.
Outbreaks difficult to control
The largest of the three hospital outbreaks was at the Royal Brompton Hospital in London. The outbreak began in April 2015 and involved 50 patients, 22 identified with infection and 9 with candidemia. The outbreak proved difficult to control, despite enhanced infection control interventions. Environmental sampling showed persistent presence of the fungus around bed space areas.
The type of multidrug resistance that's been observed in C auris has not been seen in other species of Candida. C auris also differs from other types of Candida in its ability to persist on hospital surfaces and spread between patients, although the precise mode of transmission had not yet been identified.
According to the report, results from the PHE Mycology Reference Laboratory indicate that very few multidrug-resistant C auris strains have been found in the United Kingdom, but all isolates are resistant to fluconazole, with variable resistance to polyenes (roughly 20% for amphotericin B) and echinocandins (approximately 10%).
In an updated guidance for management of C auris, PHE recommends isolation of all infected or colonized patients in a single room; use of personal protective equipment (gloves, aprons, and gowns) by healthcare workers and strict adherence to standard precautions, including hand hygiene; screening of close contacts in all hospital units that have ongoing infections or colonization and for all patients coming from other affected hospitals; and a terminal cleaning once infected or colonized patients have been discharged.
PHE says its National Infection Service is working closely with hospital microbiologists and clinicians to identify risk factors for C auris infection and colonization, and that its Biosafety Investigation Unit is investigating the fungicidal activity of different disinfectants and antiseptics.
See also:
Aug 11 PHE Health Protection Report
Aug 15 Reuters story
Aug 2017 PHE guidance